
Can you build a meaningful NHS career without becoming a doctor or nurse?
Yes, and becoming a Clinical Coder is one of the clearest ways to do it. Clinical coders work behind the scenes, but their role is essential. Their work shapes how hospitals record care, measure activity, plan services, and report what happens during treatment. In a data-driven health system, accuracy matters, and so does this role.
Interest in clinical coding in the UK continues to grow. For the right person, it offers a rare combination of medical knowledge, analytical thinking, structure, and steady progression without requiring a traditional clinical degree. If you value detail, logic, and precise work, it is a strong career option.
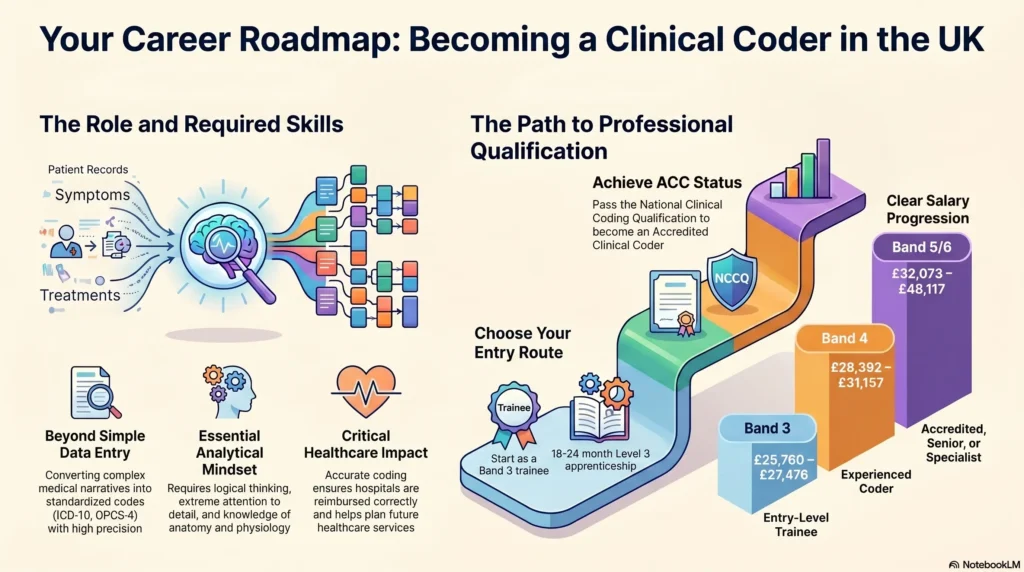
The entry path is more accessible than many expect. In the NHS, people often start in trainee roles, learn ICD-10 and OPCS-4 classifications, complete formal training, and work towards the National Clinical Coding Qualification (NCCQ). A Level 3 apprenticeship route is also available in England.
This guide explains the role, pathway, salary progression, and real day-to-day work.
What Clinical Coding Actually Is
At its simplest, clinical coding is the process of turning information from patient records into standardised clinical codes. In NHS hospital settings, diagnoses are coded using ICD-10, while procedures and interventions are coded using OPCS-4. NHS Digital explains that these classifications are used for statistical and epidemiological analysis and for reimbursing hospitals for the care they provide.
That technical description is accurate, but it does not quite capture what the work feels like. A clinical coder is not just moving words into boxes. The job involves reading medical notes carefully, working out what the record actually confirms, applying national rules correctly, and making sure the coded result reflects the patient’s episode as accurately as possible. Newcastle Hospitals describes coders as recording clinical information about every admitted patient and investigating the patient journey from start to finish.
This is why the role often surprises people. On paper, it sounds administrative. In practice, it sits somewhere between healthcare knowledge, analytical work, and regulated information management. That mix is exactly what makes the NHS clinical coder role so distinctive.
Why This Career Matters More Than It Looks
Many people only discover clinical coding careers in the UK after searching for healthcare office jobs, NHS information roles, or alternatives to patient-facing work. Once they find it, the appeal becomes obvious. It offers specialist work, a defined progression route, recognised qualifications, and a clear connection to how healthcare is measured and managed. That combination gives the role real staying power. This is an inference, but it is strongly supported by NHS careers guidance, trust career pathways, and current vacancies.
The role matters because coded data is used for much more than filing. Trust career pages and NHS-linked sources point to service planning, benchmarking, audit, epidemiology, research, and payment. When coding is accurate, hospitals can make better use of the information that flows from patient care. When coding is weak, the data becomes less dependable.
So, although clinical coders are not usually visible to the public, their work shapes how care is understood inside the system. For someone who wants meaningful work without a bedside role, that is a strong reason to take this profession seriously.

What a Clinical Coder Does Day to Day
The daily reality of the job is one of the most important parts to understand, because this is where curiosity either grows or fades. A clinical coder typically works through medical records, discharge summaries, consultant notes, test results, and procedure records to identify the diagnoses and treatments that need to be coded. If anything is unclear, they may need to contact clinicians or other staff to clarify the documentation before coding the episode properly.
That means the work is detailed, but not necessarily repetitive in a dull way. One record may be straightforward. The next may involve several co-existing conditions, a complex procedure history, or unclear terminology that needs careful judgement. NHS staff case studies describe regular contact with consultants, nursing staff, and ward teams when records need clarification.
In broad terms, a clinical coder’s day usually involves reviewing documentation, identifying diagnoses, assigning procedures, checking standards, entering data into approved systems, and supporting the wider quality of clinical information. Those steps sound neat when written down, but in reality, they demand concentration, precision, and consistency. That is why the role suits people who enjoy solving structured problems rather than rushing through quick tasks.
More Than Data Entry
This is the point many beginner articles fail to make clearly enough. Clinical coding is not simple transcription. A coder has to understand the classifications, apply the rules, and interpret the record correctly within national standards. The work calls for discipline and judgement, not just keyboard speed.
The Skills That Matter Most
If you are researching how to become a clinical coder in the UK, it helps to stop thinking only in terms of courses. Employers are not just looking for a study. They are looking for a certain type of candidate.
The NHS careers site says you will usually need a good basic education, with GCSEs or equivalent in maths, English, and science, and it also highlights the importance of computer skills. Beyond that, it points to qualities such as logical thinking, problem-solving, attention to detail, and teamwork.

What makes this more interesting is how trust case studies expand on that picture. Newcastle staff describe the need for medical terminology, anatomy, physiology, disease process knowledge, and analytical ability, alongside good communication with clinicians and other healthcare professionals. That gives you a much more realistic sense of the role.
A strong future clinical coder is usually someone who can stay calm with detail, work accurately for long stretches, and learn specialist language without getting overwhelmed by it. If that sounds like you, you are already much closer to the right profile than someone who only likes the idea of an office-based NHS job.
How to Become a Clinical Coder in the UK
Most people enter clinical coding through a trainee route and build from there. The usual path is to start in a trainee post, learn the standards in practice, complete the Clinical Coding Standards Course, and work towards the NCCQ over time.
The pathway becomes easier to understand when broken into stages:
| Stage | What This Usually Involves | Why It Matters |
|---|---|---|
| Build the Right Foundation | Start with a good base in English, maths, science, and general IT confidence. An interest in healthcare terminology and records also helps. | Clinical coding depends on careful reading, attention to detail, and accurate work with digital systems. |
| Learn What the Role Actually Is | Understand what clinical coders do in NHS settings and how ICD-10, OPCS-4, and coding standards are used. | This helps you apply realistically and shows employers you understand the profession. |
| Target Entry Routes | Apply for trainee clinical coder roles or the Level 3 Clinical Coder apprenticeship where available. | Most beginners enter through supported training routes, not as fully trained coders. |
| Train in the Workplace | Work with patient records under supervision and learn how to apply coding rules correctly. | This is where the role becomes real and practical. |
| Complete Formal Standards Training | Attend the Clinical Coding Standards Course and trust-based development. | This gives structure and supports accurate coding. |
| Work Towards the NCCQ | Progress towards the National Clinical Coding Qualification. | The NCCQ is the main recognised benchmark in NHS clinical coding. |
| Keep Developing | Continue with refresher training and more advanced coding work. | Progress depends on staying current, accurate, and confident. |
In practice, these stages often overlap rather than happen in a perfectly neat order. But as a realistic picture of how most NHS clinical coding careers develop, this is the clearest way to understand the route from beginner to qualified professional.
Training, Qualifications and the NCCQ
This is where many articles blur together beginner learning and formal professional progression. They should be kept separate.
A short course in medical terminology, anatomy, or healthcare administration may help you prepare for applications. It can improve your confidence and help you understand the language of the role. But the qualification that really matters in NHS clinical coding is the NCCQ. IHRIM describes it as the nationally recognised quality standard that provides independent assurance of competency in the use of clinical classifications and in applying associated rules, conventions, and national clinical coding standards.
That is why the NCCQ is such an important milestone in a clinical coding career UK pathway. It marks the difference between being interested in the field and having your competence recognised to a national standard. Successful candidates can use the post-nominal letters ACC, meaning Accredited Clinical Coder.
There is also continuing development after qualification. Current senior roles often ask for evidence of refresher training and up-to-date standards knowledge, which reflects the fact that this is a profession built on current rules and consistent quality. You do not qualify once and stop learning.
Trainee Route or Apprenticeship Route?
Both routes exist, and both can lead into the profession, but they are not the same.
The trainee route remains a common NHS entry pathway. Trusts recruit beginners into Band 3 or development roles, then support them through standards training, supervised experience, and later qualification milestones. Current trainee adverts show that trusts may offer hybrid working later in the pathway, but usually only after an on-site training period or after specific milestones are completed.
The apprenticeship route is more formally structured. Skills England lists the Clinical Coder apprenticeship as Level 3, with a typical duration of 18 to 24 months, and notes that apprentices without Level 2 English and maths will need to achieve that level before completing the end-point assessment.
For most beginners, the practical answer is not to pick one in theory, but to search for both in practice. The best route is often the one you can actually access.
Clinical Coder Salary UK and Career Progression
If you are checking clinical coder salary UK, the strongest benchmark is the NHS Agenda for Change structure in England. The 2026/27 pay scales published by NHS Employers show the following annual ranges.
| Band | Annual Salary |
|---|---|
| Band 3 | £25,760 to £27,476 |
| Band 4 | £28,392 to £31,157 |
| Band 5 | £32,073 to £39,043 |
| Band 6 | £39,959 to £48,117 |
That matters because many older pages still use outdated salary figures. Current vacancies support the idea that trainee roles often begin around Band 3, while more advanced, qualified, specialist, trainer, or leadership roles can move through Bands 5 and 6 depending on responsibility and accredited status.
Career progression is one of the profession’s most underrated strengths. Newcastle case studies and current NHS roles show movement into senior coding, team leadership, training, audit, and specialist functions. So, while many people discover clinical coding through entry-level searches, the role itself does not have to remain entry-level for long.
How to Get Your First Clinical Coding Job
This is the point where many readers need practical advice, not just background. The strongest approach is to tailor yourself to what live NHS roles actually ask for.
That means shaping your CV around accuracy, record-keeping, confidentiality, attention to detail, digital systems, and any sign that you are comfortable with structured information. If you have experience in healthcare administration, medical records, audit support, data quality, or document-heavy environments, those details matter. Even if the job title was different, the underlying skills can still be highly relevant. This is an inference from current adverts and person specifications, but it is a grounded one.
It also helps to show that you understand what the role involves. A candidate who can explain ICD-10, OPCS-4, coding standards, and the importance of accurate healthcare data will almost always feel more credible than someone who only says they want a stable NHS office job.
One more thing is worth saying clearly. Beginners often assume remote work will be available immediately. Current vacancies show that hybrid and remote working can absolutely exist in clinical coding, especially for experienced or accredited coders, but trainee roles usually involve more supervision at the start. That is not a drawback. It is simply part of how the profession is developed properly.
What Many Beginner Guides Miss
The first thing many guides miss is the emotional side of the role. The apprenticeship standard notes that coders may come across disturbing information in records and must always handle sensitive patient data appropriately. So, while this is an office-based profession, it still calls for maturity, discretion, and resilience.
The second thing they miss is how much of the job rests on judgment. A classification system may sound fixed, but real records are not always neat. That is why experienced coders remain important. Current senior and trainer roles still emphasise quality, standards, mentoring, and complexity, which suggests the profession is not simply being erased by automation.
The third thing they miss is that this can be an excellent long-term fit for the right kind of person. If you enjoy order, problem-solving, and the quiet satisfaction of getting complicated things exactly right, clinical coding can feel far more rewarding than its low-profile image suggests.

Is Clinical Coding a Good Career Choice?
For the right person, yes. It offers a specialist role inside the NHS, clear development routes, recognised qualifications, and work that has a real effect on how healthcare is recorded and understood. That combination makes it one of the more interesting hidden careers in the system.
It will not suit everyone. If you dislike prolonged concentration, detail-heavy tasks, or learning technical language, the job may feel demanding. But if you want a structured healthcare career with intellectual challenge, stable progression, and real value behind the scenes, becoming a Clinical Coder is a strong path to consider.
Get valuable training, UK-focused support, and the skills employers want. No experience needed.
Join 50+ graduates who landed tech jobs with our industry-focused training programme designed for beginners.
Explore Now - Our Job Ready ProgrammeFrequently Asked Questions (FAQs)
How Do I Become an NHS Clinical Coder?
Most people start in a trainee or entry-level NHS coding role, then build knowledge of medical terminology, ICD-10, OPCS-4, and coding standards while working towards the NCCQ.
What Does a Clinical Coder Do in the UK?
A clinical coder reviews patient records and converts diagnoses, procedures, and treatment details into standardised codes used for audit, planning, research, and hospital reimbursement.
Do I Need a Degree to Become a Clinical Coder?
No. You do not usually need a degree. NHS employers focus more on a solid general education, strong IT skills, accuracy, and the ability to work carefully with detailed information.
Which Certification Is Best for Medical Coding in the UK?
For NHS clinical coding, the key qualification is the National Clinical Coding Qualification (NCCQ). It is the main recognised benchmark for professional competence in this field.
How Much Do NHS Clinical Coders Get Paid?
NHS clinical coder pay follows Agenda for Change bands. In England for 2026/27, Band 3 is £25,760 to £27,476, while more advanced roles can progress through Bands 4, 5, and 6.
Can I Get a Clinical Coding Job With No Experience?
Yes. Many NHS trusts recruit trainee clinical coders and provide structured development. Foundational knowledge helps, but you can enter the profession through beginner-friendly roles.
Will AI Replace Clinical Coders?
AI may change parts of the work, but skilled coders are still needed. NHS coding depends on standards, interpretation, judgment, audit, and quality checks, especially in complex cases.
All Courses
Personal Development
Employability
Career Bundle
Management
Free QLS Certificate
IT & Software
Business
Technology
Health & Care
Quality Licence Scheme Endorsed Courses
Health & Safety
Training
Job Ready Programme
Marketing
Design
Accounting & Finance
Health and Fitness
Healthcare and Medical
Animal Care
Psychology
Microsoft Office
Teach & Education
I.T
HR and Leadership
Counselling and Therapy
Teaching & Child Care
Electrical & Electronics
Health and Social Care
Food Nutrition
Law
programming
Administration & Office Skills
Accounting
Education
Engineering
Cooking & Baking
Language
Law & Criminology
QLS Bundle
Office Skills
Photography
Awareness
Finance
Lifestyle
Diet and Nutrition
Makeup & Beauty
Therapy
Sports
First Aid
Accounting & Bookkeeping
Mathematics
Excel
Web Design
Diet and Fitness
Top Rated Course
Counselling
Agriculture
General Education
Biotechnology
Networking & Design
Audit
Economics
Lifestyle & Recreational
Adobe Photoshop
Travel and Tourism
Categories
Awarded By










